Make patient care experience AND patient satisfaction your practice super powers
Make patient care experience AND patient satisfaction your practice super powers
Last week I shared the story of a healthcare service experience that really challenged the perception of care that the patient received. When the experience as well as the clinical outcomes underperformed, questions of safety, personalisation of care and willingness to recommend or revisit the practice arose. It highlighted the importance of care experience quality and patient satisfaction with outcomes in practice reputation.
A 2024 systematic literature review in the Journal of Economic Surveys confirmed that patient satisfaction functions as a competitive advantage with direct links to financial performance in healthcare.¹ Satisfied patients are more willing to follow treatment plans, maintain ongoing provider relationships, and recommend the practice, behaviours which are tied to retention and revenue stability.²
A separate systematic review of 157 studies identified the three dominant drivers of satisfaction globally as: medical care quality, communication, and waiting time.³
With service delivery variables heavily influencing satisfaction, the “patient experience” cannot be left to individual personality, moods, or goodwill.
Patient care experience must be operationalised, and humanised
Care experience excellence does not happen in isolation. It emerges when your practice intentionally shapes the conditions for exceptional care.
Systems create the conditions.
Reliable, designed processes make the care journey predictable and safe for patients. Systems ensure that the basics never depend on memory or busyness: introductions, role clarity, medication checks, written instructions delivered at the right cognitive moment, after-hours escalation pathways, proactive follow-up scheduling, and service recovery protocols.
Team engagement delivers it at every touchpoint.
Engaged teams communicate better, show respect and empathy, and create consistent human connection, all of which research identifies as drivers of satisfaction and loyalty.³ Extending the focus to understand how delivering care also impacts your team - what aspects of care energise them and which elements they find challenging - also provides valuable insight into where support can be given.
Continuous improvement embeds it in culture.
Experience excellence is not static. It’s built through feedback loops, measurement, and iteration. When you capture patient feedback (formal surveys, complaints, compliments, informal signals) and treat it as operational intelligence, you reduce repeat failures and strengthen trust over time. Patient satisfaction surveys aren’t just for retrospective analysis; they can reliably predict quality improvement trajectories at an organisational level.⁴4
This is also where sustainability becomes visible: patient experience and employee experience move together. Burnout, disengagement, and poor teamwork don’t just hurt your workforce, they degrade the patient’s experience and safety perception.
Where is your practice positioned in the excellence/satisfaction matrix?
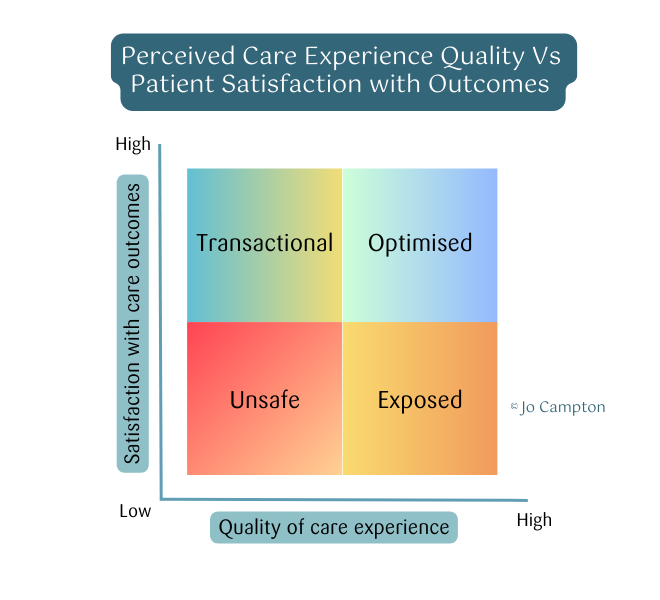
UNSAFE
Care experience quality deteriorates and outcomes follow. Safety incidents rise, satisfaction collapses, and negative association intensifies over time. The care is unsafe and the business is un-informed about gaps in service and safety.
TRANSACTIONAL
Technical components of care carry reputation. Outcomes may be adequate, but the experience feels transactional. Competitive positioning is fragile — one service failure triggers disproportionate loyalty collapse.
EXPOSED
Care may be clinically excellent, but teams or key people carry the burden of poor satisfaction ratings due to long waits, poor communication, or absent empathy. Staff fatigue, burnout and psychosocial risk increase. The business is exposed to associated costs and poor retention.
OPTIMISED
Systemised success. The patient journey is strong across key measures of experience quality. Loyalty, satisfaction and likelihood to recommend become resilient measures of practice strength. Systems, teams and improvement mechanisms support high performance.
Where to from here?
Healthcare is an increasingly competitive market, and consumers' expectations for quality outcomes as well as service excellence drive decision-making in provider choice. At the same time, the expectation on your team to do more with less is increasing.
If you are a business owner or practice manager, which quadrant of the Experience Vs Satisfaction graph do you think your practice falls into?
Thinking about your business, are there clear processes that support human connection between your clients and your team?
Do you have core values that identify the importance of the care experience?
Is your team supported in the delivery of the care experience? Do they understand why it is so important?
Do you have a way for patients and your team to share experiences of care provision - and do you use that valuable knowledge to improve or to recognise existing excellence?
I’d love to hear your thoughts.
Yours in healthcare excellence,

